
One of the most common and impactful conditions faced by our elderly population is arthritis. This degenerative condition affects millions worldwide, making everyday tasks difficult and often painful. With the aging population growing, understanding arthritis is crucial not only for those who suffer from it but also for caregivers, family members, and society at large.
What Is Arthritis?
Arthritis, a chronic disease, is not a singular condition but rather a term encompassing joint inflammation and related diseases. At its core, arthritis involves inflammation of one or more joints, leading to symptoms like pain, swelling, and stiffness.
There are over 100 types of arthritis, but the most common among the elderly are:
- Osteoarthritis (OA): A degenerative condition where the cartilage that cushions the joints wears away, leading to pain and stiffness. It often affects the knees, hips, and hands.
- Rheumatoid Arthritis (RA): An autoimmune disorder where the body's immune system mistakenly attacks the joints, causing inflammation and damage.
- Gout: Caused by a build-up of uric acid crystals in the joints, it frequently impacts the big toe but can affect other joints.
- Psoriatic Arthritis: Tied to psoriasis, this condition can lead to swollen, inflamed joints and scaly skin patches.
Symptoms
Arthritis, though common among older adults, presents itself in various ways, and its symptoms often evolve over time. Understanding the common symptoms is the first step toward seeking appropriate medical intervention.
- Joint Pain: This is the most common symptom and can affect any joint but is typically found in the knees, hips, fingers, and lower back.
- Stiffness: A stiffness in the joints, especially upon waking up or after periods of inactivity.
- Swelling: An inflammation of the joints which can lead to warmth and redness in the affected areas.
- Decreased Range of Motion: Difficulty in moving the joint normally or reduced flexibility.
- Grating Sensation: Feeling or hearing a grating sound when the joint is moved.
- Bone Spurs: Hard lumps or bone growths that form around the affected joint.
- Fatigue: A general sense of tiredness and feeling unwell.
- Joint Deformity: Especially in cases of rheumatoid arthritis, the joints and surrounding connective tissues can become deformed if left untreated.
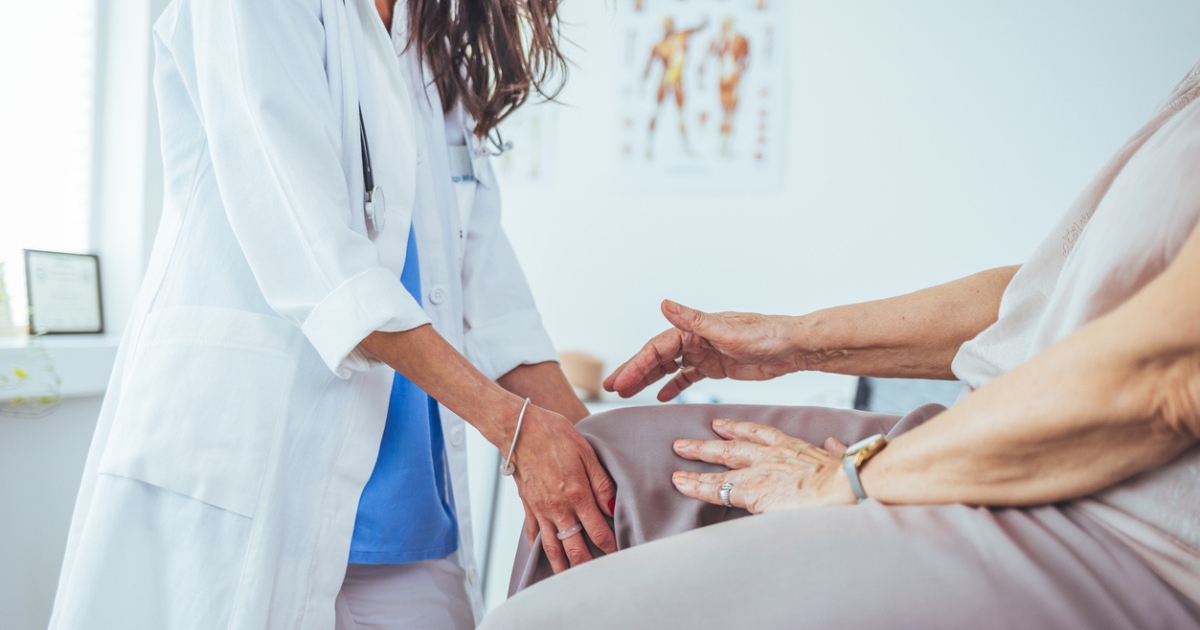
Diagnosis
As with other chronic diseases, the diagnosis of arthritis involves a combination of clinical examination and specific tests. When a patient presents with symptoms suggestive of arthritis:
- Physical Examination: A doctor will examine the joints for inflammation, redness, warmth, and will also check the range of motion.
- Laboratory Tests: Blood tests and joint fluid tests can help determine the type of arthritis one might have. For instance, certain specific antibodies are found in the blood of patients with rheumatoid arthritis.
- Imaging: X-rays can help in detecting bone spurs or other related anomalies in the joints. More detailed images from MRI (Magnetic Resonance Imaging) or CT (Computed Tomography) scans can provide a clearer picture of the joints and soft tissues.
- Arthroscopy: In some cases, a doctor might recommend a procedure where a small, flexible tube (arthroscope) is inserted into the joint to inspect and possibly retrieve small pieces of tissue for analysis.
Treatment and Management
Once arthritis is diagnosed, the focus shifts to managing symptoms and improving the quality of life for the affected individual. While there is no cure for most forms of arthritis, a range of treatments can alleviate symptoms and slow the progression of the condition.
Medications
- Analgesics: These pain relievers, such as acetaminophen or tramadol, help reduce pain but have no effect on inflammation.
- Non-Steroidal Anti-Inflammatory Drugs (NSAIDs): Like ibuprofen and naproxen, these reduce both pain and inflammation. While many NSAIDs are available over the counter, some require a prescription.
- Disease-Modifying Antirheumatic Drugs (DMARDs): Primarily used for rheumatoid arthritis, these drugs, including methotrexate and hydroxychloroquine, can slow the progression of the disease.
- Biologics: A subclass of DMARDs, biologics target specific steps in the inflammatory process. They are often more effective than traditional DMARDs but can have more potential side effects.
- Corticosteroids: These reduce inflammation and suppress the immune system. Examples include prednisone and cortisone.

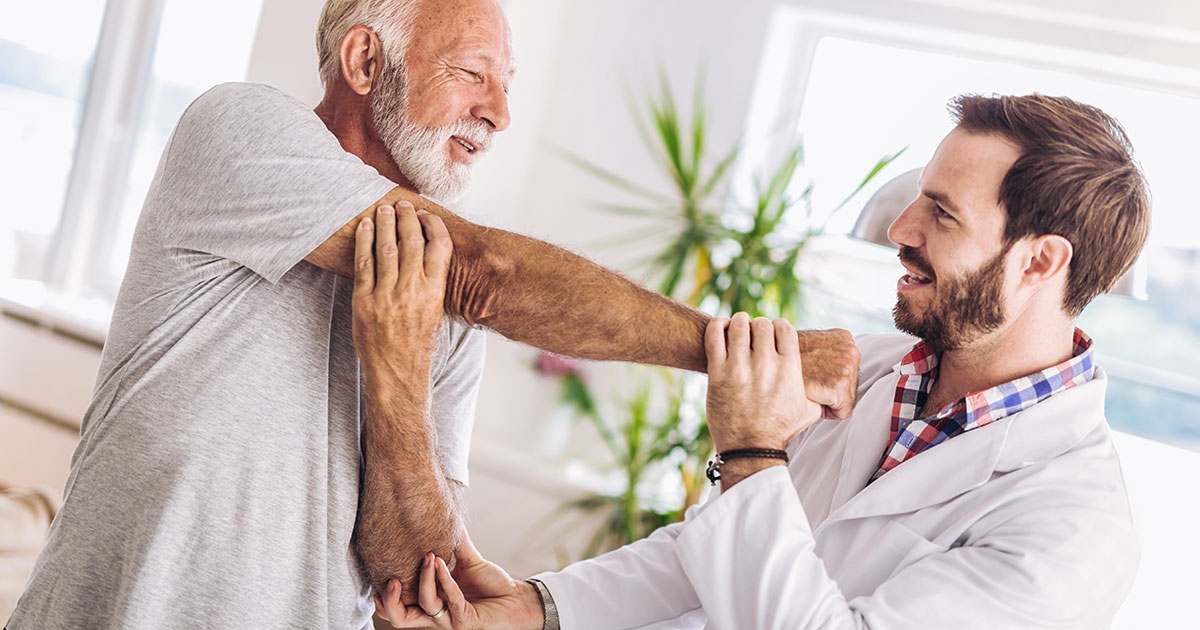
Physical and Occupational Therapy
- Physical therapy: Can provide exercises to strengthen muscles around the affected joint, increasing mobility and reducing pain.
- Occupational therapy: Teaches ways to perform everyday tasks in a manner that is less taxing on the affected joints.
Lifestyle Modifications
- Healthy Weight: Reducing body weight can significantly alleviate pressure on weight-bearing joints.
- Exercise: Regular movement helps maintain flexibility in the joints. Low-impact exercises like swimming and walking can be beneficial.
- Heat and cold therapy: Warm compresses can help ease muscle tension, while cold packs can reduce joint pain and inflammation.
- Healthy Diet: Incorporating anti-inflammatory foods like fish, nuts, and whole grains can potentially help manage symptoms.
Surgery
- Joint repair: To help improve function and reduce pain, the joint can be smoothed or realigned.
- Joint replacement: In cases of severe joint damage, the affected joint may be replaced with an artificial one, commonly done for knees and hips.
- Joint fusion: Especially used for smaller joints, the ends of the two bones in the joint are fused, leaving the bones to grow together.
Alternative Therapies
- Acupuncture: Some people find pain relief through this ancient Chinese method of inserting thin needles into specific points on the body.
- Nutritional supplements: Compounds like glucosamine and chondroitin might help in managing osteoarthritis symptoms for some people.
- Mind-body therapies: Techniques like meditation and deep breathing can help manage arthritis pain by refocusing the mind and inducing relaxation.
Keystone Health's Approach to Arthritis Treatment
At Keystone Health, we understand that arthritis is not just about joint pain – it is about living life to its fullest despite the challenges. That is why we offer a comprehensive care approach:
- Personalized Care Plans: Keystone's customized care plans ensure every patient has care tailored to their unique set of needs, symptoms, and lifestyle. These plans often combine medical treatments with lifestyle modifications to ensure the best possible outcomes.
- Chronic Care Management: Regular check-ins and consultations, either in-person or over the phone, ensure that the patient's condition is continuously monitored and any changes in symptoms or medication efficacy are addressed promptly.
- Access to Care & Care Continuity: With providers available 24/7, Keystone patients can always reach out in case of urgent needs or concerns about their arthritis management.
- Comprehensive Care Management: Keystone's staff assess not just the medical needs of arthritis patients but also their functional and psychosocial requirements. This holistic approach guarantees all facets of a patient's well-being are considered in their treatment plan.
- Alternative Therapies and Consultations: Keystone Health is open to exploring all avenues of treatment. Whether providing in-home physical therapy, discussing the potential benefits of acupuncture, or suggesting mind-body therapies, our team is here to provide informed guidance every step of the way.
Beyond the Joint Pain
Arthritis, a prevalent chronic condition among the elderly, can significantly impact the quality of life. While it presents various challenges, understanding the condition, its symptoms, and the available treatments can make living with arthritis more manageable.
Keystone Health ensures that our patients receive the personalized care, guidance, and support they need to lead a fulfilling life. With an array of treatments and interventions available, along with the undying dedication of caregivers and medical professionals at Keystone Health, there is hope for those battling arthritis to find relief and regain their zest for life.
